Surgery demands meticulous precision, focus, and steady hands. Surgeons are expected to perform at their absolute best, but what happens when they are faced with the challenge of operating with a cold? In this article, we will explore the unique difficulties surgeons face when battling a common cold while performing intricate surgical procedures. We will delve into the impact on patient care, potential risks, and the strategies employed by surgeons to navigate these challenging circumstances.
Operating Room Environment
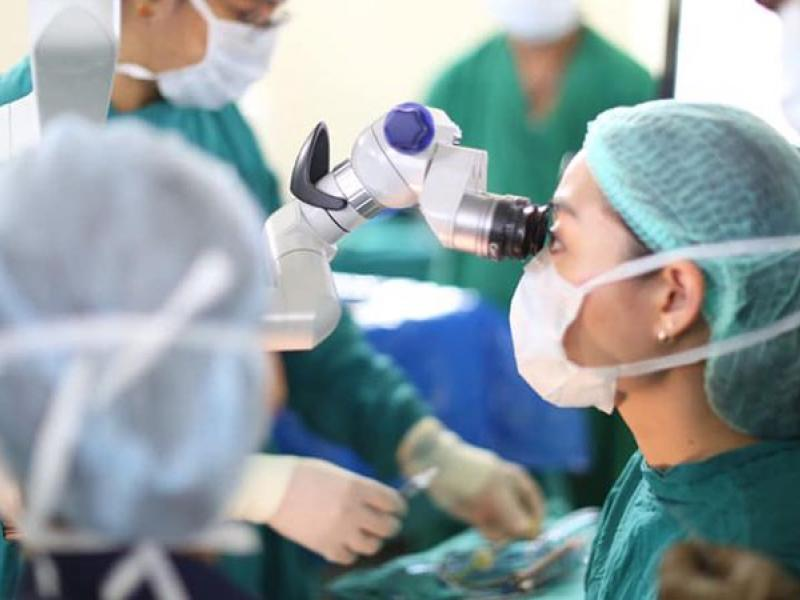
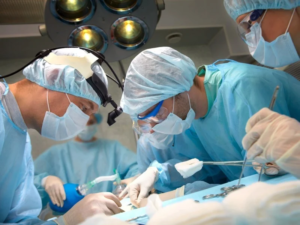
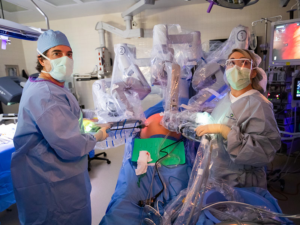
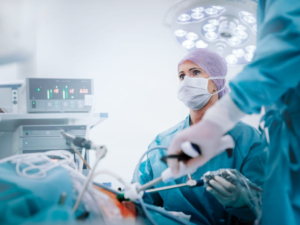
The operating room (OR) is an environment of sterility and controlled conditions. Surgeons and their support team adhere to strict hygiene protocols to minimize the risk of infections and complications. However, the presence of a surgeon with a cold introduces an additional element of concern.
Risk of Infection
While colds are typically caused by viruses, the proximity of the surgical team to the patient puts them at risk of transmitting the infection. Surgical masks and gloves offer some protection, but the possibility of inadvertent contact or aerosolization of respiratory droplets remains. Patient safety is of paramount importance, and any compromise in this regard is taken extremely seriously.
Effects on Performance
A cold can significantly impact a surgeon’s performance due to several factors. The most immediate effect is on the surgeon’s physical well-being. Symptoms like congestion, runny nose, and fatigue can make it challenging to concentrate during prolonged surgeries. Surgical masks can also impede breathing, exacerbating the discomfort.
Dexterity and Precision
Surgery requires precise manual dexterity and fine motor skills. Unfortunately, a cold can impair these abilities. Hand tremors caused by fatigue or medication can make delicate procedures even more challenging. A surgeon’s ability to maintain a steady hand may be compromised, increasing the risk of unintended tissue damage.
Decision-Making and Cognitive Function
Colds can also affect a surgeon’s cognitive abilities. Symptoms like headaches, reduced concentration, and mental fog can impede decision-making processes during complex surgeries. Given the critical nature of surgical decisions, the compromised cognitive function is a concerning aspect of operating with a cold.
Mitigating the Risks
To minimize the risks associated with operating while having a cold, surgeons take various precautions. Some common strategies include:
- Rest and Recovery: Surgeons prioritize rest and recovery to ensure they are in the best possible condition to perform surgeries. Adequate sleep, hydration, and a nutritious diet are essential for boosting the immune system.
- Medication and Symptom Management: Over-the-counter cold medications can alleviate symptoms, but caution must be exercised in choosing medications that do not impair cognitive or motor functions.
- Communication and Transparency: Surgeons must inform their colleagues and patients about their condition to allow for informed decision-making. Collaborative discussions can help assess the feasibility of postponing non-urgent surgeries.
- Enhanced Hygiene Practices: Surgeons adhere to even stricter hygiene practices, such as frequent handwashing, using hand sanitizers, and wearing double masks to minimize the risk of infection transmission.
- Team Support and Backup: In complex cases, surgeons may seek the assistance of their colleagues or consider having a backup surgeon available in case their condition deteriorates during the procedure.
Conclusion
Operating with a cold poses unique challenges for surgeons. While they strive to provide the best care possible, the physical and cognitive limitations imposed by a cold can potentially compromise patient safety. Surgeons must balance their commitment to their patients with their personal well-being and the potential risks involved. By employing strategic measures, open communication, and collaborative decision-making, surgeons can mitigate these challenges and maintain a high standard of surgical care even in the face of a common cold.