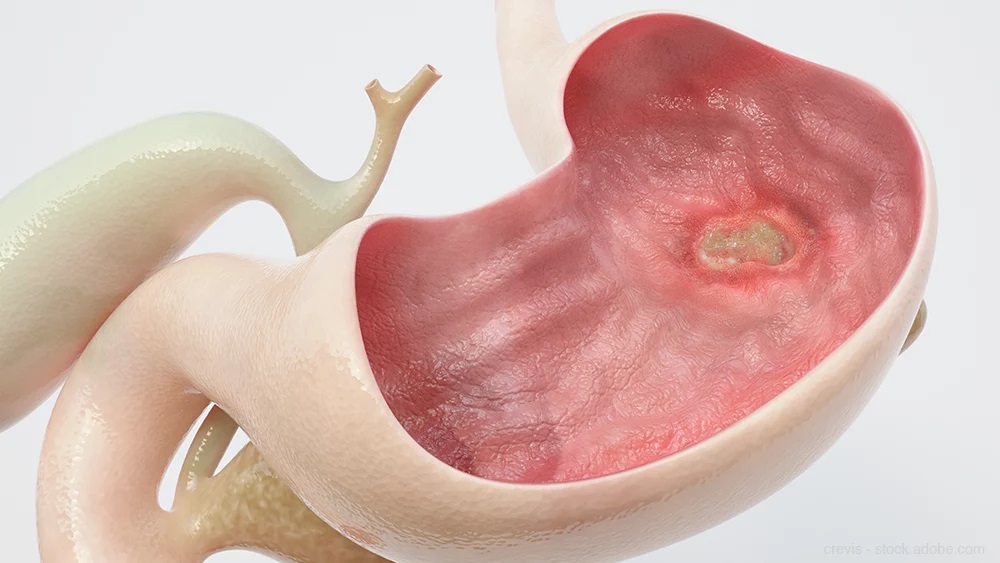
A peptic ulcer is a sore or more or less deep injury in the mucosa that covers the stomach or the first part of the small intestine. In the first case, it is called a gastric ulcer, while in the second, it is called a duodenal ulcer.
Usually, this lining or mucosa that covers the digestive tract protects it from the action of gastric acids, which are necessary for the digestion of food. However, this protection can be weakened for various reasons, which, in the long run, end up damaging the wall of the stomach or duodenum.
Who is affected?
A peptic ulcer is a relatively frequent pathology since it affects between 5{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76} and 15{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76} of the population of developed countries, also as Spain. This prevalence is even higher in developing and underdeveloped countries.
Duodenal ulcer is usually diagnosed around the age of 40. It is more common in men, while the gastric ulcer is not diagnosed until the average age of 55 and affects both sexes equally.
What causes peptic ulcers?
According to the Spanish Federation of the Digestive System, until a few years ago, it was considered that the leading cause of this pathology was precisely an excessive production of gastric acids. In fact, until the 1990s, it was considered a chronic relapsing disease (recurring in a patient); Currently, it is known to have a mainly infectious origin.
Thus, the latest research has revealed that the causes of the acids beginning to damage the walls of the stomach and duodenum are two:
- Infection by the bacterium Helicobacter payroll (H. pylori): this is a bacillus whose biological properties have allowed it to adapt to the stomach’s acidic environment. Ulcers caused by this bacterium cannot be prevented since approximately 50{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76} of the world’s population is already infected with it. However, only 10{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76} and 20{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76} of these people will develop a gastric or duodenal ulcer, and the rest will live without problems with the infection.
- Prolonged use of nonsteroidal anti-inflammatory drugs (NSAIDs) (the best known are acetylsalicylic acid or ibuprofen): these drugs are often used to alleviate chronic processes such as pain or normal rheumatic processes or acute processes such as acute inflammation or fever. Sometimes, or used in excess, they can cause unwanted side effects such as a gastric or duodenal ulcer. Contrary to what happens with lesions caused by Helicobacter payroll bacteria, this type of peptic ulcer can be prevented.
What factors increase the risk of suffering from it?
Several factors increase the risk of developing a peptic ulcer. We can note the following:
Genetics. Various studies confirm that peptic ulcer is up to three times more frequent in first-degree relatives of people who already suffer from this lesion.
Infection by the bacterium Helicobacter pylori. H. pylori is present in 90{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76}-100{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76} of cases of duodenal ulcers and 60{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76}-80{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76} of gastric ulcers. This bacillus can be transmitted from person to person or faecal-oral, so the hygienic-sanitary conditions of the patient are decisive. For this reason, this infection is more frequent in undeveloped countries, affecting almost 80{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76} of people.
Regularly take nonsteroidal anti-inflammatory drugs (NSAIDs). Many studies confirm the relationship between the intake of these drugs and the two types of peptic ulcer, although the risk of lesions from this cause increases if the person has several factors:
- History of ulcer or ulcer complication.
- Age over 60 years.
- High dose of NSAID drugs.
- Simultaneous use of corticosteroids or anticoagulants.
- Coexistence of severe disease or gastroesophageal reflux.
- Helicobacter pylori infection.
Smoking. The relationship between ulcers and tobacco is very clear. Smokers are twice as likely to suffer from this disease than the rest of the population. In addition, tobacco delays the healing of the ulcer, favours the reappearance of the disease, can reduce the effectiveness of treatment and increases complications.
What are your symptoms?
In many cases, ulcers are asymptomatic and are only detected when the first complication occurs. In general, the most common symptom is pain or burning in the upper part of the abdomen, which presents typical characteristics that lead to suspicion of the disease: it is located at the level of the pit of the stomach, it appears two or three hours after the meals. It calms down with the intake of food or antacids. It can last minutes to hours and sometimes even wake the affected person during the night. These discomforts affect the patient for more or less prolonged periods and with periods free of pain.
Likewise, many patients debut with bleeding (vomiting blood or expelling black and sticky stools or with black dots). This appearance is more frequent in the elderly and more so if they take NSAIDs.
In addition to pain, other symptoms of the ulcer patient are:
- Nausea.
- Vomiting.
- Change in body weight.
- Anorexia.
What complications can peptic ulcers cause?
In order of frequency, the most frequent complications are bleeding, perforation and penetration into neighbouring organs, and narrowing of the stomach outlet (pyloric stenosis).
Digestive bleeding is the most common complication.
Perforation and penetration into neighbouring organs. The ulcer penetrates all the stomach or duodenum layers and reaches the peritoneal cavity and, in some cases, through neighbouring organs such as the pancreas or liver. This problem, which can lead to death, occurs in 5{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76} of affected people and is more common in men. Bleeding and perforation are related to NSAID intake.
Pyloric obstruction or stenosis. The healing and retraction of a duodenal ulcer can narrow the pylorus – the opening that leads from the stomach to the small intestine – and make it difficult for the stomach to empty. It is more common in older men, although it is a rare complication. And all complications are more frequent in smokers.
On the other hand, it is believed that suffering from peptic ulcers increases the probability of suffering from gastric cancer. According to the World Health Organization, the H. Pylori bacteria increases the risk of stomach cancer. In this sense, the risk factors for this disease include the following aspects:
- Helicobacter pylori stomach infection.
- Chronic gastritis (inflammation of the stomach).
- Pernicious anaemia.
- Intestinal metaplasia (a condition in which the usual lining of the stomach is replaced by the cells that line the intestines).
- Familial adenomatous polyposis (FAP) or gastric polyps.
- Eat a diet high in salt, smoked foods, and a few fruits and vegetables.
- Eating food that was not prepared or stored correctly.
- Being old or male.
- Smoking cigarettes.
- Having a parent or sibling who had stomach cancer.
How is it diagnosed?
The most common test to diagnose an ulcer is gastroscopy. This exam allows visualizing the walls of the stomach and duodenum, as it is performed with a flexible tube inserted down the throat and has a built-in camera. This technique allows, in addition to confirming or ruling out the presence of a peptic ulcer, Helicobacter pylori bacteria or an infection, to take biopsies (tissue samples) to determine the benign or malignant nature of the lesion. Although it is an invasive technique, it is not painful, as it is performed under sedation.
Another possible diagnostic test is contrast radiography, although it is less reliable than endoscopy and does not allow biopsies to be taken.
Likewise, Helicobacter pylori infection can be confirmed as the cause of the ulcer with an expired air sample or C13 urea breath test. The specialist may also order haemoglobin or faecal occult blood test.
Can peptic ulcers be cured?
Yes, both in the case of ulcers caused by Helicobacter pylori infection and those related to nonsteroidal anti-inflammatory drugs. In this second case, the treatment consists of suspending the intake of the previous medications and administering PPIs (proton pump inhibitors) such as omeprazole, lansoprazole or pantoprazole to the ulcerative person for several weeks to achieve ulcer healing.
In the case of Helicobacter pylori infection, the most effective treatment combines three medications (a PPI and two antibiotics) for seven days. The disease is eliminated in 80{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76}-85{d6b3193afd8499af2f28ac17c1a3778c4e6c8819d5d73c7dc9806223890cfc76} of cases. In the rest of the patients, a second rescue treatment consisting of a PPI drug and three antimicrobials is applied.
Surgical or radiological procedures may be necessary in the case of ulcers that do not heal or severe complications, such as severe bleeding or perforation.
Ten tips to prevent and cope with peptic ulcer
Following a series of healthy recommendations can help prevent peptic ulcer disease and, if the injury has already occurred, better cope with the symptoms and promote healing. And it is essential to know that if you have a gastric or duodenal ulcer, you can lead an everyday life.
- Forget tobacco.
Or at least reduce its consumption since smoking is one of the main risk factors for the appearance of peptic ulcers and can also delay healing and reduce the effectiveness of treatment.
- Eat everything, but with common sense.
Contrary to popular belief, peptic ulcer sufferers do not need to follow a special diet; instead, they should restrict the foods that most often cause pain, burning or other symptoms.
- Moderate the consumption of coffee and spicy foods.
Although these foods are not direct causes of ulcers, they can worsen them, so people suffering from this ailment should not abuse them.
- Attention to alcohol.
The same happens with the consumption of this substance: its relationship with the appearance of peptic ulcers has not been proven, but it can favour the formation of complications. Limit alcohol consumption to no more than two drinks per day.
- Antacids and milk are good allies.
Although neither cures peptic ulcers, both can relieve symptoms and make this ailment more bearable.
- Do not abuse aspirin and nonsteroidal anti-inflammatory drugs (NSAIDs).
Once the disease develops, this type of medication should be suppressed or taken restrictive, but healthy people should also moderate their intake and take only the recommended doses. Paracetamol can be a good alternative, although, in any case, you should never self-medicate.
- Don’t overdo the use of stomach protectors either.
Sometimes we tend to take stomach protectors too quickly and on our own; however, it must be the doctor who tells us the use of these medications.
- Monitor the appearance of your stools.
Especially in older people, sticky black stools or stools with blackheads are the first sign of digestive bleeding caused by ulcers. Therefore, its appearance must be monitored as a preventive measure.
- Go to the doctor when you perceive the first symptoms.
Contrary to what has been thought for a long time, the ulcer can be cured, in most cases, with oral treatment. The specialist will make the correct diagnosis of our disease and will prescribe the appropriate medications for each patient.
- Strictly comply with the medical prescription.
To achieve the eradication of the infection and the total healing of the ulcers, it is essential that the patient strictly apply the administration guidelines dictated by the specialist. You must also follow the treatment to the end. The success rate largely depends on it.